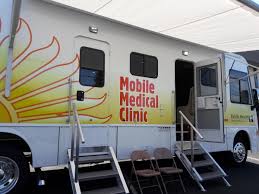
Seattle Considers Mobile Injection Van
The “Head Tax” isn’t the only major controversy in Seattle politics these days.
Seattle City Council is forging ahead with plans for a publicly funded “safe injection” facility.
I’m just getting up to speed on the discussion here, and wanted to pull together a post that summarizes where we’ve come from, what we know about such approaches done elsewhere, and where we stand today. I’ll be adding to this list of resources over time.
Present View: Skeptical, at Least as Planned
I’m sympathetic to the harm-reduction model. If we could only isolate the users to those who are already here, and had confidence it would be well run with detox pathways in-place and extra policing in the area, and if we had a good handle on other aspects of homelessness, I could see supporting spinning up such a new effort.
But the more I peruse the existing, often conflicting body of evidence and try to apply it to what SCC is pursuing, the more skeptical I become. Given tremendous mismanagement of municipal efforts by the council, I also think the lens of our taxpayer-funded services needs to shift to a stack-ranked model — does safe injection pioneer work rise to the level of “must do now?” given fiscal constraints?
I am also concerned about funding yet another “magnet” policy which will likely draw people from the region and the country to Seattle who need more services when we are already overcapacity serving our own. Further, as evidenced in Vancouver, any solution here needs full cooperation of the police, cooperation from the local community (where?), extra police resourcing (funds) to be able to “surge” around the facility, as well as clear obligations on the part of those who do use, such as helping us understand whether it’s drawing people regionally. And it’s not at all clear these days, after all the expense that Vancouver’s harm reduction strategy is actually working.
The Beginnings: 2016
2016 was the year that the Seattle City Council started seriously moving ahead with ideas around safe-injection. SCC has taken its cue from the harm reduction model that was first implemented in North America in Vancouver BC.
March 21, 2016
A key milestone in this effort was March 21st 2016, when the SCC’s Human Services & Public Health Committee heard an overview of Vancouver’s Insite by Liz Evans, former nurse and one of the founders of Insite in Vancouver. The presentation and Q&A which followed are well worth a watch:
CM O’Brien asks a question about location at about 41:00. Evans says “You won’t even get people to go eight blocks – you need to be where drug users are.”
Fast Forward to June, 2018
While California may get the nation’s first “safe injection” site this summer, Seattle is on course to fund and deploy one of the first-in-the-nation taxpayer-funded “safe injection” facilities. But it looks like it won’t be a building.
The City Council has recently shifted its approach from a fixed location to a “fixed-mobile” facility, which is in essence a very large outfitted recreational vehicle (RV) which will be used to provide a “safe space” for injection. The “fixed” moniker refers to the fact that it’ll return every day to the same location. The location itself is currently TBD.
Here’s a good overview of where we are as of mid June 2018 from Q13. CM Mosqueda advocates for moving ahead with the $350,000 van purchase even though location has not yet been determined and vetted with neighboring community, and many other important details aren’t nailed down:
The specific plan, including who qualifies for treatment, whether there is anything asked of participants, what data is tracked, how physically the injection and post-injection effects will be handled in the context of a vehicle with limited capacity, and treatment pathways offered off of addiction are unclear to me.
I’m still learning about the evolving plans; perhaps someone in the comments could direct me to the specific plan in development. How do we measure the results and impact on the neighborhood as compared with costs? What constitutes “success”?
Further reference on studies:
- Research papers on Semantic Scholar (“insite injection”).
Projected Cost
On the cost side of the ledger, the budget appears to be:
- $350,000 for van
- $1.5 million to outfit it
- Ongoing operating costs: $2.5 million per year
Lots of Questions
- How many injection stations will this van have?
- Where will this be located?
- How much “throughput” is expected here on a typical day? Presumably it’s not large enough to have the detox within the facility, as it is in Vancouver. (At Insite, “detox” is upstairs.) Maybe the plan is to have the detox in the van, but that will limit the throughput considerably.
- What data do we have from Insite about the success of going from path from addiction to clean?
- How will the drugs be purchased?
- Which drugs specifically — heroin, fentanyl… others?
- Will this be a regional “magnet” for more addicts to come to our region? How will we measure and know? (Will clients be asked for ID’s and point of origin? Will non-locals’ use of this facility be time-limited in any way?)
- We are repeatedly told that we don’t have enough money by the City Council. So what makes this the “highest and best use” of funds?
- Are non-civic funding sources sought at all?
- Do users get checked against, say, outstanding arrest warrants?
- What extra policing plans will there be as this is deployed?
What Can We Learn from Insite in Vancouver? Data is Mixed.
As noted above, the approach is being modeled after Vancouver’s Insite facility, the first such “safe consumption” site in North America.
The question: “Is Vancouver working?” has answers on both sides, and the data seems quite ideologically driven. In 2016, Evans cited “over 40 peer reviewed studies.” In particular, Evans mentions a study by the Lancet which shows a reduction in deaths in the surrounding area by 35%, but another follow-on study notes serious errors were made in reaching that conclusion. Evans also notes that there is no increase in crime in the area, something which as been quite disputed by Vancouver’s police department itself.
Those in favor of publicly-funded injection sites may site this study as written up by Macleans: “The Science Is In. And Insite Works.” Those opposed might find Tristin Hopper’s opinion in National Post more suitable: “Vancouver’s Drug Strategy Has Been a Disaster: Be Very Wary of Emulating It.”
Crime does appear to be growing in the Insite Neighborhood:

And Vancouver is now ranks among North America’s highest for opiod overdose deaths.
And grim anecdotes abound:
[Vancouver’s Safe Injection “Insite” Facility] sits smack in the middle of an eye-popping outdoor drug market and shooting gallery. Here’s a snapshot: a urine-soaked alley, directly behind Insite. A man squats on the broken pavement, poking a needle into an open, bleeding wound in one arm. Another man stands nearby, moaning, eyes glazed, a sharp protruding from his wrist. Next to him, a woman holds a small cosmetics mirror in front of her face. She’s not applying makeup; she’s pushing a needle into her neck.
Back on Hastings, right next to Insite, a thin man in a dirty orange t-shirt and ragged blue jeans sits on the sidewalk, cross-legged, pulling small folds of heroin from a plastic bag. He’s handing the drugs to a steady stream of customers. No one bothers to disguise or conceal their transactions.
Some buyers walk straight into Insite, where they will give a name—pseudonyms aren’t discouraged—to a receptionist, and sit inside a waiting area until they are called into a large space behind a locked door. Once there, they will pick up fresh, sterile equipment, sit at one of 13 mirrored, stainless steel booths, and fix. Nurses may sit or stand next to the users as they inject. This takes an average of 20 minutes, says Tim Gauthier, one of Insite’s two clinical coordinators.
— from “Vancouver Supervised Injection Struggles with Fentanyl”
While I do think the “harm reduction” model should not be dismissed out of hand, my inclination is first, before we have a clear understanding of why this is a good idea, do no harm.
Before we establish a program to help scaffold more injection, we really need clear data on the results. What’s the policing plan? What’s the plan to measure results? What’s the plan, if any, to check the ID’s of those who are using against, say, arrest warrants?
One statistic often cited by Insite supporters is that there have been no deaths inside the Insite facility, and Seattle has had many people die on its streets of overdose. Will a mobile lab have enough capacity to make the same claim? Will people exit these vehicles high?
Citizens Speak Out
On social media, some comments have included:
- “There are already hundreds of mobile injection RV’s parked around the city.”
- “When you are actually funding injection vans, you know that your first priority is not to reduce homelessness.”
- “Last year we had 169 people die on our streets. If this helps reduce it, it’s worth it. Life is precious.”
Cautionary words from Vancouver Police Union about Supervised Injection Sites
“So that wherever these facilities are located, the negative impact of the associated drug use can be managed so other citizens aren’t negatively impacted,” says Vancouver Police Union President Tom Stamatakis. “I think when you look at illegal drugs and activities associated to that you need to look at it more holistically. You can’t just focus on harm reduction, you also have to focus on prevention, education and enforcement.” Stamatakis agrees police here have had to deal with a lot more because of supervised injection sites.
While Neil Arao, Insite Manager reports “There hasn’t been an increase in crime rates, there hasn’t been an increase in violence or anything in the community,” other reports are that the Vancouver Police had to add 65 additional police officers to the area, because it tends to attract an increase in regional crime. Are such extra-policing plans being put forward, and at what cost?
Branding: Call It A “Public Health Clinic”
One thing is clear — the effort to sell this idea on a wary public is not lost on City Councilmembers. Formerly called “Community Health Engagement Locations” (CHELS), that term is now deemed doubleplus-ungood. On April 19 2018, Councilmembers Bagshaw and Juarez both emphasized that branding is important, for a very wary (and weary) public:
“I don’t think we’re doing a bait and switch with people.” – CM Juarez
More reading
- Experts Challenge Vancouver’s Safe Injection Stats
- Seattle considers mobile safe injection van
- Cautionary words from Vancouver Police Union about supervised injection sites
- Why Some US Cities Are Opening Safe Spaces for Injecting Heroin
- Vancouver’s Supervised Injection Site Struggles with the Rise of Fentanyl
- Is Vancouver’s Safe Trug Use Site a Good Model for Seattle?
- Seattle Moving Forward with Safe Mobile Injection Site
- Drug War Facts